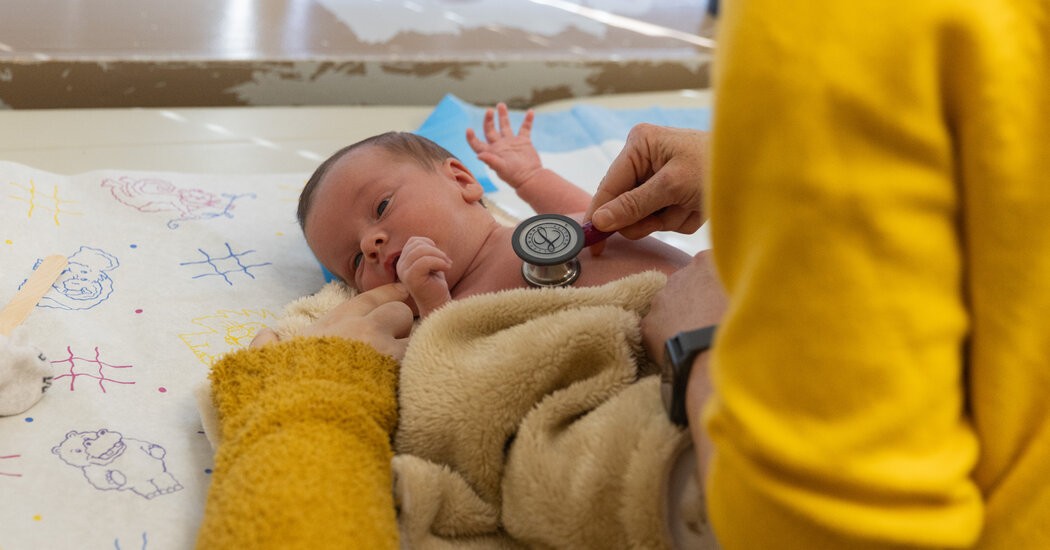
Pediatricians across the United States are increasingly navigating complex conversations with parents hesitant to vaccinate their children, a trend fueled by widespread misinformation and mistrust in medical institutions. These discussions are often delicate, requiring clinicians to balance patient health advocacy with respectful understanding of parental concerns.
The Rising Tide of Vaccine Hesitancy
Historically, vaccine skepticism remained on the fringes of American public health. However, the COVID-19 pandemic dramatically shifted this landscape. The rapid development and rollout of COVID-19 vaccines, coupled with associated mandates, reinvigorated anti-vaccine sentiments and deepened hostility toward the medical establishment.
Clinicians like Dr. Alissa Parker, a pediatric nurse practitioner in Ashland, Kentucky, now regularly encounter parents who decline routine childhood vaccinations. In one case, parents of an 11-day-old infant had already refused the hepatitis B vaccine at birth and planned to continue rejecting other recommended immunizations. Dr. Parker and other medical professionals must tread carefully, offering information without pressure, as direct confrontation often exacerbates mistrust.
Why This Matters: A Public Health Challenge
The increase in vaccine hesitancy poses a serious threat to public health. Vaccines are a cornerstone of preventative medicine, protecting not only individuals but also communities through herd immunity. Declining vaccination rates risk outbreaks of preventable diseases like measles, whooping cough, and polio, which can have severe consequences, particularly for infants and immunocompromised individuals.
The situation is complicated by the sheer volume of misinformation online. Parents often encounter unsubstantiated claims about vaccine safety, conspiracy theories, and false narratives that erode confidence in medical science. Countering this misinformation requires not just scientific data but also empathetic communication that addresses underlying fears and uncertainties.
Navigating Difficult Conversations
Pediatricians are adapting their approach to these conversations. Instead of forceful persuasion, many prioritize building trust, providing clear, evidence-based information, and addressing specific parental concerns. The goal is to empower parents to make informed decisions, even if those decisions differ from medical recommendations.
However, the emotional and professional toll on clinicians is significant. Dealing with deep-seated mistrust while upholding ethical obligations to protect children’s health creates a challenging and emotionally draining work environment.
Ultimately, combating vaccine hesitancy requires a multi-faceted approach: improved public health communication, robust fact-checking initiatives, and continued efforts to rebuild trust in the medical community. Without these measures, the resurgence of preventable diseases remains a real and growing threat.